- KASBN International, Lahore, Pakistan
- 0092-42-35763338
- 0092-42-35878200
- info@kasbnmedical.com
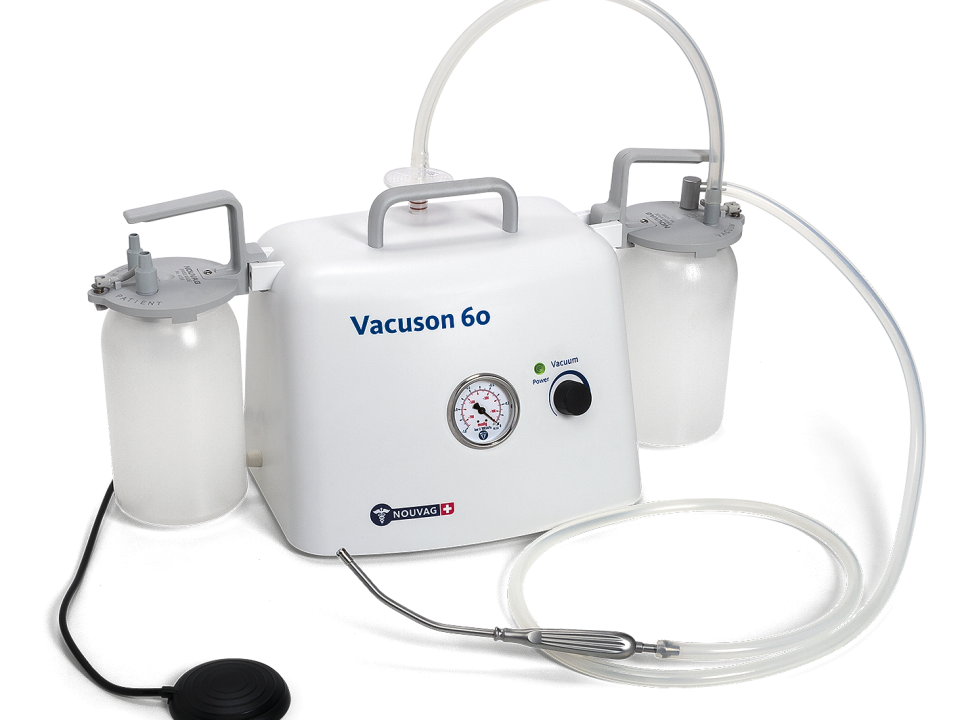
Vacuson 60
October 31, 2017Case
Code pink in labour and delivery, and you are the only doctor in the hospital tonight…
(This is an update of a prior version of this post based on the newest 2015 ILCOR/AHA/ERC guidelines)
The biggest changes are:
We no longer intubate and suction for meconium. The resuscitation proceeds identically whether or not meconium is present
Heart rate is monitored using ECG leads, rather than the classic palpation of the umbilicus
CPAP is added as an option for laboured breathing or persistent cyanosis
The first 30 second assessment has been removed because it was unrealistic. The goal is to just get an initial assessment and initial maneuvers done in the first minute.
My approach
Call for help. Hopefully the code pink activated the pediatrician already. I like to bring a second ED doc if they happen to be around, if just for moral support.
Make sure the proper equipment is available. The baby should be in a warmer. You need appropriately sized lines and tubes. The unusually small doses take longer to draw up, so now is a good time to get a spare nurse to start drawing up the correct epinephrine dose.
The first step of neonatal resuscitation asks three questions to determine if the baby is ok: Is this a term gestation, is there good tone, and is the baby breathing or crying? Presumably at least one answer was no, which is why you are at a code pink.
Identify yourself and ask where the team is in the algorithm (it probably took you some time to run up a few flights of stairs). We will assume you got there immediately.
Stimulate, position, warm. Dry with towels, position and clear the upper airway, stimulate with gentle rubbing or heel flicks. (In the premature infant, less than 28 weeks, do not towel dry as the skin is very fragile. Instead, maintain warmth by wrapping in plastic or placing the child in a plastic bag.) Make sure that the radiant warmer has been turned on, because the baby needs to be kept warm whether or not further resuscitation is required.